|
Overview
Pain in arch of foot, a very common problem for millions of people worldwide who are suffering from this ailment every single day. Whether it's arch pain, heel pain, bunion pain, big toe pain, little toe pain or anything else in between, sore feet are no fun! It's no denying that if your feet aren't right, you feel out of sorts. In this article you will discover the possible causes of the pain in the arches of your feet and common treatments and solutions. Often linked with heel pain, pain in the arch of the foot is very common, particularly in those that spend a lot of time on their feet and those that play sports regularly. Causes At the other end of the spectrum, yet within the same category of congenital flat foot, exist several rare, more severe forms of flat foot. These severe conditions include Vertical Talus, Congenital Calcaneal Valgus, and Tarsal Coalitions - all of which are more rigid (no arch with or without weight on the foot) and definitely symptomatic. Luckily, these are much less common, but can usually be identified by specialists at the time of presentation and treated appropriately. The second category, acquired flat foot, develops over time, rather than at birth. Many different factors can contribute to the development of flat feet. These include the types of shoes a child wears, a child's sitting or sleeping positions, compensation for other abnormalities further up the leg, or more severe factors such as rupture of ligaments or tendons in the foot. Very commonly, the reason for flat feet is that the foot is compensating for a tight Achilles tendon. If the Achilles tendon is tight, then it causes the foot to point down, or to plantarflex (as occurs when stepping on the accelerator of your car). Even minimal amounts of plantarflexion can simulate a longer leg on that particular side, assuming that the other foot is in the normal position. The body therefore tries to compensate by pronating, or flattening out the arch, thereby making up for the perceived extra length on the affected side. Symptoms Experiencing chronic pain of any kind can lead to feelings of fatigue, irritability and even depression. Friends may joke about having 'tired dogs' after a long day, but this is completely different from your experience if arch pain has begun to impact your life on a daily basis. You may dread getting out of bed in the morning and wonder how you're going to get through a work day without having to limp home at the end of it. Diagnosis The medical practitioner will examine how the muscles of your foot function. These tests may involve holding or moving your foot and ankle against resistance; you may also asked to stand, walk, or even run. Pain caused by movements may indicate the cause of the pain. The nerves in the foot will be tested to make sure no injury has occurred there. An x-ray, MRI, or bone scan of the foot and arch may be taken to determine if there are changes in the makeup of the bone. Non Surgical Treatment Consult a doctor to diagnose the condition and determine the cause. If revealed to be plantar fasciitis, please refer to our article on that injury for further information. Generally arch pain is easy to treat, with the most effective method of treatment being the placement of arch supports in the shoes. This counteracts the strain placed on the arches by biomechanical errors, causing them to cease stretching excessively. A specialist can recommend the inserts suitable to your needs, which will depend on the shape of your arches. These supports should lessen your symptoms within days. If pain is severe you should refrain from running activities until it subsides to avoid risking an aggravation of the injury. To maintain fitness, alter your training program temporarily to be focused on low-impact sports like swimming. Applying ice to the affected area should assist in reducing pain and swelling.  Surgical Treatment In adults, the most common cause of collapse is due to the posterior tibial tendon tear. In such cases, the tendon must be repaired and a second tendon may be added to the posterior tibial tendon for strength and added support. If the foot is found to be very flat, bone realignment procedures or possible bone fusion procedures may be used to realign the foot. If the calf or Achilles tendon are found to be tight, they may be lengthened to allow better motion at the ankle and less arch strain. The forefoot may also be in a poor position and stabilization of the arch may be necessary to increase forefoot contact to the ground. Stretching Exercises Inchworm. Stand with your weight on one foot. Raise the metatarsal heads of the unweighted foot while you pull its heel closer to your toes. Next, raise your toes toward the ceiling, and then relax your whole foot with it flat on the floor. Your foot should move like an inchworm across the floor. Reps 6-7 for each foot. Horsepawing. Stand with your weight on one foot and the other foot slightly in front of you. Raise the metatarsal heads on the front foot. Lift your heel ever so slightly off the ground, maintaining the raised metatarsal heads, and pull your foot toward you so that it ends up behind you. Return this foot to the starting position in front of you. You should really feel this one in your arch. Reps. 6-7 for each foot. Toe pushups. Sit in a chair with your feet resting on the floor. Raise your heel as high as you can while keeping your toes flat on the floor. This is the starting position. Using your toe muscles, roll your foot upward until the weight of your foot is resting on the ends of your toes, like a dancer standing on point in toe shoes. Roll back down to the starting position. Reps. 10-20 for each foot. Sand scraping. Pretend you are at the beach standing in loose sand. Use your big toe to pull sand inward toward your body, with your little toe off the ground. Then use your little toe to push it away, with your big toe off the ground. Reps. 10 for each foot. Now reverse the exercise: pull the sand inward with your little toe and push it away with your big toe. Reps. 10 for each foot. Overview
Most flat feet usually are generally not painful, specially individuals flat feet noticed in children. Throughout the actual adult acquired flatfoot, pain occurs simply because soft tissues (tendons along with ligaments) happen to be torn. Your deformity progresses or even worsens because once your important ligaments and also posterior tibial tendon are lost, absolutely nothing may take their own location to carry up the actual arch with the foot. Your painful, progressive adult acquired flatfoot affects females four times as frequently as men. The idea occur in middle for you to older get older people with a suggest chronilogical age of 60 years. The Majority Of people who develop the situation currently have flat feet. a alter occurs in a foot the location where the arch begins to flatten greater than before, with pain and swelling developing about the inside with the ankle. Exactly why this event occur in some people (female more than male) in assistance of in one foot remains poorly understood. Contributing factors enhancing the likelihood of adult acquired flatfoot are generally diabetes, hypertension, along with obesity. 
Causes There are generally numerous leads to regarding acquired adult flatfoot, which includes fracture as well as dislocation, tendon laceration, tarsal coalition, arthritis, neuroarthropathy, neurologic weakness, and iatrogenic causes. the most common trigger regarding acquired adult flatfoot will be posterior tibial tendon dysfunction. Symptoms Some symptoms of adult acquired flat foot are usually pain over the inside in the foot along with ankle, pain that will raises using activity, along with problems strolling for too long intervals involving time. An Individual might expertise difficulty standing, pain about the outside the ankle, as well as bony bumps around the the surface of the foot and also inside your foot. you might also have got numbness along with tingling in the feet as well as toes (may outcome through big bone spurs putting stress on nerves), swelling, a big bump on the sole of the foot and/or an ulcer (in diabetic patients). Diabetic patients ought to put on a properly fitting diabetic shoe don in order to avoid these complications from happening. Diagnosis The diagnosis associated with posterior tibial tendon dysfunction and also AAFD will be generally made from any combination of symptoms, physical exam and also x-ray imaging. Your area involving pain, model of the particular foot, overall flexibility of the hindfoot joints and also gait most might aid your own physician result in the diagnosis as well as assess how advanced the situation is. Non surgical Treatment Flatfoot may become treatable with a assortment associated with methods, which includes modified shoes, orthotic devices, a new brace or even cast, anti-inflammatory medications as well as restricted steroid injections, rest, ice, and physical therapy. Within severe cases, surgery may become necessary. 
Surgical Treatment If original conservative therapy of posterior tibial tendon insufficiency fails, surgical treatment is actually considered. Operative treatment regarding stage 1 disease involves release of the particular tendon sheath, tenosynovectomy, debridement in the tendon using excision regarding flap tears, and also repair involving longitudinal tears. The short-leg strolling cast is actually worn regarding three weeks postoperatively. Teasdall and also Johnson reported total relief involving pain within 74% associated with 14 patients undergoing this treatment program with regard to stage 1 disease. Surgical debridement regarding tenosynovitis inside first stages is believed to become able to probably avoid progression associated with disease to become able to later on stages regarding dysfunction. Overview
Arch pain occurs with an inflammation of the plantar arch or fascia. It is the thick membrane that covers and supports all the muscles of the sole of the foot from the heel bone to the base of the toes that is called plantar arch. When this membrane pulls excessively (constant strain), pain developes in the arch of the foot or heel. 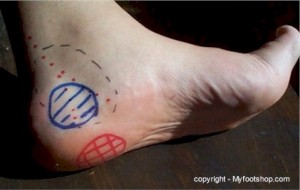
Causes If the feet are exposed to damp conditions for prolonged periods, you can develop Trench Foot. Most commonly associated with World War One, it now tends to be seen in builders, hikers or festival goers. Trench foot causing numbness and bottom of foot pain. With Trench Foot, the sole of the foot turns a white/grey colour and you may develop pins and needles or numbness. Other symptoms include pain in bottom of foot and swelling. If left untreated, you can develop blisters and permanent nerve damage which can lead to the need for amputation. Treatment and prevention aim to reduce the dampness around the foot and ensure good foot hygiene. Slowly rewarming the feet and using special products in a foot bath really helps reduce the damage and foot arch pain from Trench Foot. Symptoms If you've ever seen your footprints in the sand and they looked more like bricks than feet, then you probably have flat feet. Simply stated, a flat foot is a foot that does not have an arch when standing. In the medical world, flat feet are associated with "pronated" feet. Pronated is merely the term used to describe the position of the foot when it is flexed upward (dorsiflexed), turned away from the body (abducted), and the heel is rolled outward (everted), all at the same time. A certain amount of pronation is required for normal walking, but too much pronation is often considered a foot's "worst enemy." Over time, excessive pronation can lead to many unpleasant problems including heel pain, bunions, hammertoes, shin splints, and even knee, hip, or back pain. In fact, one orthopedic surgeon discovered that 95% of his total knee replacement patients and 90% of his total hip replacement patients had flat feet. An easy way to tell if you pronate too much is to take a look at your athletic shoes-excessive wearing of the inside heel (arch side of the shoe) as compared to the outside is a classic indication of excessive pronation. Diagnosis Flat feet are easy to identify while standing or walking. When someone with flat feet stands, their inner foot or arch flattens and their foot may roll over to the inner side. This is known as overpronation. To see whether your foot overpronates, stand on tiptoes or push your big toe back as far as possible. If the arch of your foot doesn't appear, your foot is likely to overpronate when you walk or run. It can be difficult to tell whether a child has flat feet because their arches may not fully develop until they're 10 years of age. Non Surgical Treatment In mild cases of flatfoot the first line of treatment is often custom orthotics. In patients with a flexible deformity, supporting the arch with a custom arch support will take the strain off the joints and muscles, bringing the heel into a corrected position. Wider shoe gear may be prescribed to accommodate foot pain and motion and stretching exercises to decrease stiffness and stress on the foot. In cases of severe collapse, especially if the patient is not a good surgical candidate or has a mild tear, a brace may be made to accommodate the foot and ankle, thus supporting the arch and ankle. 
Surgical Treatment Patients with adult acquired flatfoot are advised to discuss thoroughly the benefits vs. risks of all surgical options. Most procedures have long-term recovery mandating that the correct procedure be utilized to give the best long-term benefit. Most flatfoot surgical procedures require six to twelve weeks of cast immobilization. Joint fusion procedures require eight weeks of non-weightbearing on the operated foot, meaning you will be on crutches for two months. The bottom line is: Make sure all of your non-surgical options have been covered before considering surgery. Your primary goals with any treatment are to eliminate pain and improve mobility. In many cases, with the properly designed foot orthosis or ankle brace, these goals can be achieved without surgical intervention. Stretching Exercises Stretching your calf and Achilles tendon may also help as a tight Achilles can make your foot overpronate. To stretch your calf and Achilles tendon, step forwards with your left leg and bend it, with your right leg straight and both feet pointing forwards. Push your right heel into the ground while keeping your right leg straight; you should feel the stretch at the back of your right leg, below the knee. Hold the stretch for 15 to 30 seconds and repeat with the opposite leg. Repeat the stretch two to four times on each leg, and repeat the overall exercise three to four times a day. Overview
The arch of the foot is a very complex structure, consisting of multiple bones and ligaments. Most causes of arch pain are related to the anatomy of the arch and the types of physical activity that you perform. For example, a classic set up for arch pain is people who engage in lots of high impact exercise (such as running) while wearing a type of athletic shoe that does not properly support their type of foot arch. If you notice that the twinges of pain you have are most commonly associated with or immediately after exercise, you might want to visit a good athletic shoe store to make sure you are wearing the right kind of shoe. Another cause of arch pain is plantar fasciitis. The plantar fascia is a tough tissue structure that holds the bottom part of the arch in place. The fascia often becomes inflamed and sore, usually as a result of repetitive motion (for example, very common in those who stand on their feet for work). The pain is often noticeable first thing in the morning and worse with activity. In addition to wearing good arch supports and taking anti-inflammatory medications, stretching exercises are often a part of the treatment. You should see your primary care doctor to determine what is the best treatment for you. 
Causes There are a variety of causes of flat feet. Flat feet can be genetic, acquired and develop over time. Young children and teens can have no arches. Injury can lead to flat feet. Tendon problems, and arthritis can lead to flat feet. Rigid flat feet may occur from a condition called tarsal coalition, where the bones in the back of the foot are genetically fused or locked together. Symptoms People suffering from pain in the arch sometimes complain of burning or soreness on the foot sole, which is worse in the morning and after physical activity. There may also be some tenderness when pressure is applied to the sole of the foot or heel. In addition to this, patients tend to complain of more pain when they stand on tiptoe. Diagnosis In people with flat feet, the instep of the foot comes in contact with the ground when standing. To diagnose the problem, the health care provider will ask you to stand on your toes. If an arch forms,the flat foot is called flexible. You will not need any more tests or treatment. If the arch does not form with toe-standing (called rigid flat feet), or if there is pain, other tests may be needed, including a CT scan to look at the bones in the foot. MRI scan to look at the tendons in the foot. X-ray of the foot. Non Surgical Treatment Treatment for a high arch foot or Charcot Marie Tooth disorder depends on the extent of deformity and the amount of disability experienced by the patient. Depending upon the symptoms, treatment may include. Changing the shoes. Special orthotic supports (devices that support, adjust, or accommodate the foot deformity). Cushioning pads. Foot and ankle braces or surgery. 
Surgical Treatment There are two types of bone procedure for flat feet, those where bone cuts and bone grafts are used to alter the alignment by avoiding any joint structures, or joint invasive procedures (called fusions or arthrodeses) that remove a joint to reshape the foot. With joint fusion procedures, there are those procedures that involve non-essential joints of the foot versus those that involve essential joints. All bone procedures have their place in flat foot surgery, and Dr. Blitz carefully evaluates each foot to preserve as much motion and function while obtaining proper and adequate alignment. In many cases a flat foot reconstruction involves both soft tissue procedures and bone procedures to rebuild and restore the arch. There are several joints in the arch of the foot that can collapse - and these joints are non-essential joints of the foot. This does not mean that they do not have a purpose, but rather become inefficient is providing a stable platform for function. As such, locking these non-essential non-functioning joints into place is commonly recommended. These joints are fused together with screws and/or plates. A heel bone that is no longer in proper position and pushed outwards away from the foot can be corrected with a bone cut and realignment procedure, so long as the displacement is not too significant. A benefit of this surgery is that it keeps the back portion of the foot mobile, and helps the surrounding tendons work for efficiently in maintaining the arch. In certain flat feet, the foot is deviated outwards and away from the midline of the body. Sometimes, this is due to the outer portion of the foot being shorter than the inner portion. Here bone graft can be added to the outer edge of the foot to lengthen the foot to swing the foot over into a corrected position. This procedure is most commonly performed in children and young adults. A bone graft is inserted into the top part of the arch to realign a component of the flat foot, medically known as forefoot varus or medial column elevatus. The back part of the foot (called the rearfoot complex) can be the cause (or source) of the flat foot or the simply affected by the flat foot foot. In simple terms, the back part of the foot can be made to flatten out due to arch problems - and vica versa for that matter. Dr. Blitz specifically identifies the cause of the flat foot as this will determine the best treatment plan, as each flat foot needs to be evaluated individually. The rearfoot is made up of three joints, and depending on the extent and most importantly the rigidity of these joints, they may require fusion to restore alignment. When all three joints require fusion - this call is a triple arthrodesis. For completeness, isolated fusion of any of the three joints can be performed (such as subtalar joint arthrodesis, talonavicular arthrodesis, and calcaneaocuboid joint arthrodesis). The medical decision making for isolated fusions is beyond the scope this article, but Dr. Blitz tries to avoid any rearfoot fusion for flexible feet because these are joints are essential joints of the foot, especially in younger people. Those in severe cases, it may be advantageous to provide re-alignment. Prevention The best way to prevent plantar fasciitis is to wear shoes that are well made and fit your feet. This is especially important when you exercise, walk a lot, or stand for a long time on hard surfaces. Get new athletic shoes before your old shoes stop supporting and cushioning your feet. You should also avoid repeated jarring to the heel. Maintain a healthy weight. Stretch when you feel a tightening of the ligament that runs along the bottom of your foot. Stop impact sports when symptoms first occur. Stretching Exercises Strength training and stretching can help avoid injury and keep your feet free from pain. Stretching should focus on the bottom of your foot to loosen tissues and tight ligaments surrounding your arch. The easiest way to do this is by grabbing a towel and sitting on the floor. You can do this while you catch up on the news in the morning, or when you get home from work. Put one leg out in front with your foot flexed up. Loop the towel around the ball of your foot and gently pull your toes towards you. Hold for thirty seconds and then repeat 3-4 times before switching feet. Overview
Plantar Fasciitis is a common condition that involves degenerative changes (wear and tear) of the thick fibrous band of tissue that runs from the heel bone beneath the arches through to the ball of the foot. Plantar Fasciitis can be caused by a range of factors including: high impact exercises, excessive body weight, hormonal changes and/or foot biomechanics (foot alignment with weight bearing including high arches or flat feet). 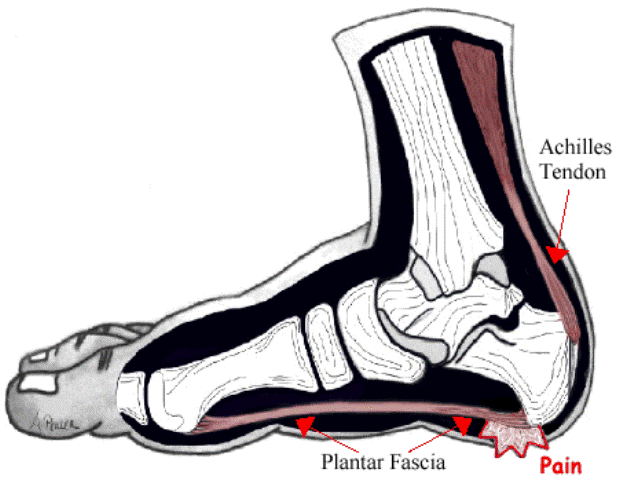
Causes There are a number of other medical conditions that can cause foot arch pain such as diabetes, arthritis and obesity. These can affect the position and strength of the bones, muscles, ligaments and tendons, leading to bottom of foot pain. It sounds simple but footwear plays an important role in how our feet feel. Foot arch pain is commonly caused by ill-fitting shoes, especially ones with little arch support or that are too tight. Footwear is particularly important if you are going to be spending long periods on your feet or for sporting activities such as running. Shoes should be supportive, comfortable, cushioned, provide the appropriate level of arch support and be the correct width. Symptoms Experiencing chronic pain of any kind can lead to feelings of fatigue, irritability and even depression. Friends may joke about having 'tired dogs' after a long day, but this is completely different from your experience if arch pain has begun to impact your life on a daily basis. You may dread getting out of bed in the morning and wonder how you're going to get through a work day without having to limp home at the end of it. Diagnosis Magnetic Resonance Imaging (MRI) can show tendon injury and inflammation but cannot be relied on with 100% accuracy and confidence. The technique and skill of the radiologist in properly positioning the foot with the MRI beam are critical in demonstrating the sometimes obscure findings of tendon injury around the ankle. Magnetic Resonance Imaging (MRI) is expensive and is not necessary in most cases to diagnose posterior tibial tendon injury. Ultrasound has also been used in some cases to diagnose tendon injury, but this test again is usually not required to make the initial diagnosis. Non Surgical Treatment What remedies work best depends on the source of your pain. Stretches help tightened, overused muscles to relax, and exercises help weakened ones to regain the strength they need to hold your foot in its proper place. Prescription orthotics add extra support and help your arch more efficiently distribute weight. Changing your shoes to ones that better cushion and brace your foot also help. Generally flatfoot pain doesn?t require surgery, unless the problem was caused by a torn tendon. You may then need a procedure to repair the damaged tissue and realign your arch. 
Surgical Treatment The main goal of surgery is to reduce pain and improve function. It may also reduce other injuries such as repeated ankle sprains and broken bones. Surgery may be considered if there is no relief with physical therapy, changes in shoewear and/or changes in activity. Some patients will also have tendon problems, ankle weakness and foot fractures. These patients may require other procedures to address related problems. If you have medical problems that make surgery unsafe, any infections or blood vessel disease, cavus foot surgery may not be appropriate. The surgical procedures involved with the correction of the cavus foot are varied. Theses may include correction of the bony deformity, ankle looseness and the muscle imbalances that cause the deformity. The goal is to provide a foot that evenly distributes weight along both inside and outside edges. A variety of incisions may be needed to perform the procedures related to the correction of the cavus foot. Prevention Arch pain occurs when the plantar fascia becomes worn down due to constant strain or excessive exercising. This may be caused by increasing your running or hiking mileage too fast, wearing inadequate footwear, lack of stretching, running on steep hills, standing on your feet for too long and abnormal anatomy such as flat foot. Stretching is an important exercise that should not be overlooked because the tightness or lack of tightness of the joints in the foot can also cause pain in the arch. Stretching Exercises People with flexible feet who develop fallen arches may benefit from foot strengthening exercises, notes the Nicholas Institute of Sports Medicine and Athletic Trauma. Standing on a towel in bare feet and grasping the material with the toes is an easy foot-strengthening exercise that can be done at home. Standing on one leg while arching and releasing the foot may also prove useful. Doctors may prescribe gentle stretching exercises for the foot and ankle tendons. Overview
Most people with flat feet have a condition that is referred to as a flexible flat foot. This is caused by excessive flexibility within the joints and ligaments of their foot and is often hereditary. This results in an over pronated (rolled in) position and is exaggerated by mechanical misalignment of the foot. This can be a very destructive position for the foot to function in and can cause a wide variety of foot, leg and lower back conditions. The appearance of flat feet may vary from foot to foot. Generally there is a collapse of the medial (inside/middle) long arch of the foot. This may occur mildly where the arch height drops slightly or can be a large movement that results in the entire length of the arch resting on the ground. The twisting and misalignment of the foot that occurs with arch collapse can cause excessive wear and tear of the foot joints and eventually pain. Causes Having low or no arches is normal for some people. In these cases, flat feet are usually inherited and the feet are fairly flexible. Occasionally, flat feet can be caused by an abnormality that develops in the womb, such as a problem with a joint or where two or more bones are fused together. This is known as tarsal coalition and results in the feet being flat and stiff. Flat feet that develop in later life can be caused by a condition that affects the joints, such as arthritis, or an injury to a muscle, tendon or joint in the foot. Symptoms Flat feet don't usually cause problems, but they can put a strain on your muscles and ligaments (ligaments link two bones together at a joint). This may cause pain in your legs when you walk. If you have flat feet, you may experience pain in any of the following areas, the inside of your ankle, the arch of your foot, the outer side of your foot, the calf, the knee, hip or back, Some people with flat feet find that their weight is distributed unevenly, particularly if their foot rolls inwards too much (overpronates). If your foot overpronates, your shoes are likely to wear out quickly. Overpronation can also damage your ankle joint and Achilles tendon (the large tendon at the back of your ankle). See your GP if you or your child has flat feet and your feet are painful, even when wearing supportive, well-fitting shoes, shoes wear out very quickly, feet appear to be getting flatter, feet are weak, numb or stiff, Your GP may refer you to a podiatrist (foot specialist). Diagnosis The doctor will take a brief history to determine how the injury occurred. If necessary, a thorough physical exam may be conducted to evaluate for any other injuries. Taking your workout shoes to the exam may also provide valuable information to the medical practitioner. Both feet will be physically and visually examined by the medical practitioner. The foot and arch will be touched and manipulated possibly with a lot of pressure and inspected to identify obvious deformities, tender spots, or any differences in the bones of the foot and arch. Non Surgical Treatment Treatment for these injuries varies depending on the severity of the injury. Most strains and sprains can be treated with rest, ice, compression and elevation (RICE). Moderate to severe cases, however, may require some form of immobilization such as a brace or a cast. Certain injuries that don't heal within the expected time frame may require surgery. It is important to seek medical attention as soon as possible for foot and ankle injuries, especially if it is causing you to limp or there is swelling. Prompt and appropriate treatment and rehabilitation ensures the best possible recovery. 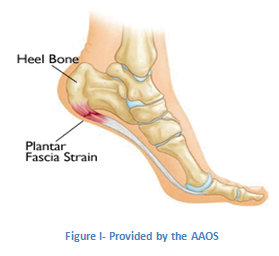
Surgical Treatment As with most surgeries, patients and physicians should consider the surgery only after other, less invasive treatments have proven unproductive. Indications for surgery include Pain. Inability to function. Failure to improve after a six-month course of specific, directed physical therapy. Failure to improve after using arch supports, orthotics, or ankle and foot bracing. Once patients are at that point, the good news is that the procedure has considerably better outcomes than more traditional flat foot surgery. In the past, surgeons would realign and fuse the three hind joints, which would cause patients to lose motion, leaving them with a significantly stiff hind foot, With these newer procedures, if the foot is still flexible, surgeons can realign it and usually restore a close-to-normal or functional range of motion in the joints. Prevention Foot and ankle injuries are common in sports, especially running, tennis and soccer. But sports enthusiasts can decrease the risk of injury by taking some precautions. Lightly stretch or better yet, do a slow jog for two to three minutes to warm up the muscles. Don't force the stretch with a "bouncing motion." The amount of time spent on the activity should be increased gradually over a period of weeks to build both muscle strength and mobility. Cross training by participating in different activities can help build the muscles. People whose feet pronate or who have low arches should choose shoes that provide support in both the front of the shoe and under the arch. The heel and heel counter (back of the shoe) should be very stable. Those with a stiffer foot or high arches should choose shoes with more cushion and a softer platform. Use sport-specific shoes. Cross training shoes are an overall good choice; however, it is best to use shoes designed for the sport. Stretching Exercises Below are two simple plantar fasciitis stretching exercises to help improve the flexibility of the muscles and tendons around the foot and ankle. Plantar fasciitis stretch taken from The Stretching Handbook. Kneel on one foot and place your body weight over your knee. Keep your heel on the ground and lean forward. In the photo to the left, the athlete is stretching the arch of her left foot. Kneel on one foot with your hands on the ground. Place your body weight over your knee and slowly move your knee forward. Keep your toes on the ground and arch your foot. In the photo to the right, the athlete is stretching the arch of his right foot. Overview

The Achilles tendon may end up being the soft tissue positioned within the heel which throughout turn connects calf muscle mass to the heel bone allowing your body to perform specific activities like rising about the suggestion toes and also pushing off when running or perhaps walking. Achilles tendon tears occur if the tendon gets in order to be torn by indicates of excessive pressure place around the area which the particular tendon can be unable to withstand. Tears are most often located when suddenly accelerating from the standing position along with as a result is frequently noticed in runners along with athletes associated with racquet sports. a tear can additionally occur when a steady force can be being place around the heel by implies of prolonged ranges involving activity and overuse however this may in addition occur as becoming a results of sudden impact as well as force towards the region widespread throughout get within touch with sports for example rugby and also hockey. Though Achilles tendon tears can vary within their severity, the rupture is the the vast majority of serious type of tear as well as involves any totally torn tendon. This particular injury is more widespread throughout patients inside their 30’s as well as 40’s. Causes Achilles tendon rupture happens in individuals that engage throughout strenuous activity, who're generally sedentary and have weakened tendons, or in those whom have had previous chronic injury for their Achilles tendons. Prior injury towards the tendon may be due to overuse, improper stretching habits, worn-out or improperly fitted shoes, as well as poor biomechanics (flat-feet). The Actual likelihood of tendon rupture can in addition be elevated with the use regarding quinolone antibiotics (e.g. ciprofloxacin, Levaquin). Symptoms Following are usually a few in the symptoms generally associated by getting an Achilles tendon rupture. Sudden, severe pain, swelling, bruising, problems walking. At times the gap might end up being felt inside the tendon. the most common ways an Achilles tendon rupture is actually diagnosed are clinical history (presenting symptoms). Thompson or Simmonds’ test, positive if when squeezing the actual calf there's no foot movement (passive planter flextion). O’Brien’s test, needles they fit to the tendon; tendon can be intact if once the foot can be moved up as well as down, your needle hub moves inside the identical direction because the toes (opposite direction in the tendon) Ultrasound as well as MRI, because these technologies involve an extra expense, they are usually employed simply to confirm the diagnosis. Diagnosis a physician typically could make this diagnosis having a good physical examination and history. X-rays usually are generally not taken. Any straightforward test of squeezing your calf muscles while lying on your abdomen should indicate if the tendon can be nonetheless connected (the foot ought to point). This particular test isolates the particular link between your calf muscle along with tendon and eliminates various other tendons which might even now allow weak movement. Any word regarding caution, Achilles tendon rupture can be often misdiagnosed as a strain as well as minor tendon injury. Swelling and the continuing power to weakly point your toes may mix up the actual diagnosis. Ultrasound as well as MRI are tests that can assist inside tough diagnosis. Based about the degree of injury, these exams can also assist inside figuring out that therapy might end up being best. Non Surgical Treatment Not every torn Achilles tendon needs an operation. recent numerous studies have proven in which even any conservative treatment, i.e. immobilizingt the leg can lead to satisfactory healing successes. This specific requires, however, the patient is actually fitted with a cast (immobilization splint) and/or a special boot for any period involving time regarding approximately 6 - 8 weeks. Right After that, the particular boot should be worn throughout your day for around two a lot more weeks. An intensive physiotherapy will begin after about about six weeks to train your calf muscles in order that the particular original coordination may be restored. running coaching in flat ground may be began once again following an additional 10 - 12 weeks. Studies show that the chance of the recurring torn tendon can be higher after a conservative treatment opposed to a operative treatment. Depending on the kind regarding treatment, regarding 10 - 15 percent regarding individuals affected may expect at a amount of point for an individual to once more have problems with a new tear of the Achilles tendon. Moreover, within the non-operated cases, we possess seen more frequently a substantial permanent weakness with the footprint, specially restricting the opportunity to be concerned in sports. 
Surgical Treatment This injury will be usually treated surgically. Surgical care adds the risks associated with surgery, there are for you to view. Following the surgery, the particular cast as well as aftercare is usually as follows. The below-knee cast (from just below the particular knee to the guidelines in the toes) is actually applied. the first cast might become applied along together with your foot positioned inside a downward direction to allow the ends of the tendon to lie closer together pertaining to original healing. An Individual may be brought back again throughout 2-3 week intervals until the actual foot may be positioned from 90 degrees for the leg in the cast. The really first 6 weeks inside the cast are usually typically non-weight bearing with crutches or just concerning any other suitable device to assist with most the non-weight bearing requirement. Right After 6 weeks inside the non-removable cast, a removable walking cast is actually started. the removable walking cast can be removed with regard to therapy, sleeping and bathing. Your time period inside the removable walking cast might need to final to possess an further 2-6 weeks. Your Current physician will review a home physical therapy plan together with you (more in this program later) that will typically start not long right after your non-removable cast will be removed. The physician might also refer you for formal physical therapy appointments. Typically, excess weight bearing exercise activities are generally kept limited regarding a minimal of 4 weeks or perhaps more. Swimming as well as stationary cycling activities could always be allowed sooner. complete healing usually takes twelve months or perhaps more. Overview

Achilles tendon ruptures commonly exist in athletic people in their 30s and 40s whilst doing activities that need sudden acceleration or perhaps changes in direction (ex. basketball, tennis, etc.). Patients typically describe a clear pain in their heel region virtually as if these folks were “struck in the again of the leg”. The Actual diagnosis of an acute Achilles tendon rupture is created upon clinical examination as x-rays will reveal the particular ankle bones being normal. the Achilles is the largest along with strongest tendon inside the body. This is actually topic for anyone to 2-3 occasions body weight during regular strolling so regaining normal Achilles tendon function will be critical. Achilles tendon ruptures may be successfully handled non-operatively, as well as operatively, but they should be treated. Surgical remedy leads to the faster recovery along using a lower charge involving re-rupture. However, surgery could be associated using extremely serious complications such as a new possible infection or wound healing problems. for this purpose non-operative treatment could end up being preferable inside many individuals, specially those patients along with diabetes, vascular disease, along with individuals who're long-term smokers. Causes The tendon typically ruptures without any warning. The idea will be most frequent within men between your ages regarding 40-50, that play sports intermittently, for example badminton as well as squash. Presently there has been possibly some degeneration inside the tendon prior to the rupture which may as well as may not have been causing symptoms. Symptoms Patients which suffer an acute rupture of the Achilles tendon often statement hearing the "pop" or even "snap." Patients usually have severe pain the rear involving the low leg near the heel. This might or may not really be accompanied by swelling. Additionally, because the function with the Achilles tendon is often to enable plantarflexion (bending the foot downward), patients often have a problem strolling or perhaps taking the stand on their toes. Diagnosis The staggering 20%-30% involving Achilles tendon ruptures are missed. Thompson (calf squeeze) test can be 96% sensitive as well as 93% sensitive. Unfortunately, several health practitioners fail to perform this simple clinical test. Ultrasound examination or even an MRI could confirm an Achilles tendon rupture. Non Surgical Treatment This situation ought for you to be diagnosed along with treated as soon as possible, since prompt remedy possibly improves recovery. A Person may require to be referred urgently to always be able to view a doctor throughout an orthopaedic department as well as accident and also emergency department. Meanwhile, if your ruptured Achilles tendon will be suspected, a person should not place any excess weight upon that foot, so do certainly not walk on it from all.Treatment options with an Achilles tendon rupture include surgical and also non-surgical approaches. The Particular decision associated with whether to move forward along with surgery as well as non-surgical treatment is situated around the severity in the rupture and additionally the patient’s health status and also activity level. Non-surgical treatment, which is typically associated using a higher charge associated with re-rupture, can be selected pertaining to minor ruptures, less active patients, along with these together with medical circumstances which avoid all of them from undergoing surgery. Non-surgical remedy involves use of the cast, walking boot, or even brace to restrict motion and permit the particular torn tendon in order to heal. 
Surgical Treatment The objective regarding surgery is always to realign both ends with the ruptured tendon to always be able to allow healing. You will find multiple processes to make this happen goal that may change from surgeon in order to surgeon. Recovery via this injury is usually very productive together with go again to full perform in approximately six months. Publish operatively casting is necessary with the use of crutches or other indicates to keep non-weightbearing pertaining to 4-8 weeks. This is followed with a course of physical therapy. Partial rupture could or perhaps may not need surgical intervention depending around the extent of injury but cast immobilization is actually a widespread requirement. Overview  The Achilles tendon is the largest tendon in the body. It connects your calf muscles to your heel bone and is used when you walk, run, and jump. Although the Achilles tendon can withstand great stresses from running and jumping, it is vulnerable to injury. A rupture of the tendon is a tearing and separation of the tendon fibers so that the tendon can no longer perform its normal function. The Achilles tendon is the largest tendon in the body. It connects your calf muscles to your heel bone and is used when you walk, run, and jump. Although the Achilles tendon can withstand great stresses from running and jumping, it is vulnerable to injury. A rupture of the tendon is a tearing and separation of the tendon fibers so that the tendon can no longer perform its normal function.Causes There are a number of factors that can increase the risk of an Achilles tendon rupture, which include the following. Youre most likely to rupture your Achilles tendon during sports that involve bursts of jumping, pivoting and running, such as football or tennis. Your Achilles tendon becomes less flexible and less able to absorb repeated stresses, for example of running, as you get older. Small tears can develop in the fibres of the tendon and it may eventually completely tear. There is a very small risk of an Achilles tendon rupture if you have Achilles tendinopathy (also called Achilles tendinitis). This is where your tendon breaks down, which causes pain and stiffness in your Achilles tendon, both when you exercise and afterwards. If you take quinolone antibiotics and corticosteroid medicines, it can increase your risk of an Achilles tendon injury, particularly if you take them together. The exact reasons for this aren't fully understood at present. Symptoms An Achilles tendon rupture is when the tendon that connects the heel bone to the calf muscle tears and the fibers separate. This happens mostly between the ages of 30 and 50, and usually is caused by sports. Symptoms of Achilles tendon rupture include the following. A pop or snap when the tendon tears. Severe pain in back of the ankle, making it nearly impossible to walk. Swelling and discoloration. Tenderness. Inability to rise on toes. A gap in the back of the ankle where the tendons are separated. Diagnosis The actual area of an Achilles tendon rupture cannot be seen on x-ray. Therefore, although x-rays are often done to rule out bony injuries in individuals with an Achilles tendon rupture these x-rays are usually normal. Diagnostic ultrasound of the tendon can be performed to assess the integrity of the tendon. Other diagnostic tests, such as MRI's, may also be required in difficult cases. Non Surgical Treatment Initial treatment for sprains and strains should occur as soon as possible. Remember RICE! Rest the injured part. Pain is the body's signal to not move an injury. Ice the injury. This will limit the swelling and help with the spasm. Compress the injured area. This again, limits the swelling. Be careful not to apply a wrap so tightly that it might act as a tourniquet and cut off the blood supply. Elevate the injured part. This lets gravity help reduce the swelling by allowing fluid and blood to drain downhill to the heart. Over-the-counter pain medication is an option. Acetaminophen (Tylenol) is helpful for pain, but ibuprofen (Motrin, Advil, Nuprin) might be better, because these medications relieve both pain and inflammation. Remember to follow the guidelines on the bottle for appropriate amounts of medicine, especially for children and teens.  Surgical Treatment Surgery for Achilles tendon rupture requires an operation to open the skin and physically suture (sew) the ends of the tendon back together, has a lower incidence of re-rupture than nonsurgical treatment. Allows return to pre-injury activities sooner and at a higher level of functioning with less shrinkage of muscle. Risks are associated with surgery, anesthesia, infection, skin breakdown, scarring, bleeding, accidental nerve injury, higher cost, and blood clots in the leg are possible after surgery. Surgery has been the treatment of choice for the competitive athlete or those with a high level of physical activity, for those with a delay in treatment or diagnosis, and for those whose tendons have ruptured again. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
July 2017
Categories |
 RSS Feed
RSS Feed
